For non-melanoma skin cancers, the diagnosis and treatment in the U.S. increased by 77 percent between 1994 and 2014. Some known risk factors for basal cell carcinoma – the most common non-melanoma skin cancer for those with European ancestry – include exposure to UV radiation, family history of skin cancer, and lighter pigmentation.
One study found that 86 percent of melanomas can be attributed to exposure to ultraviolet (UV) radiation from the sun. Approximately 90 percent of non-melanoma skin cancers are associated with exposure to ultraviolet (UV) radiation from the sun.
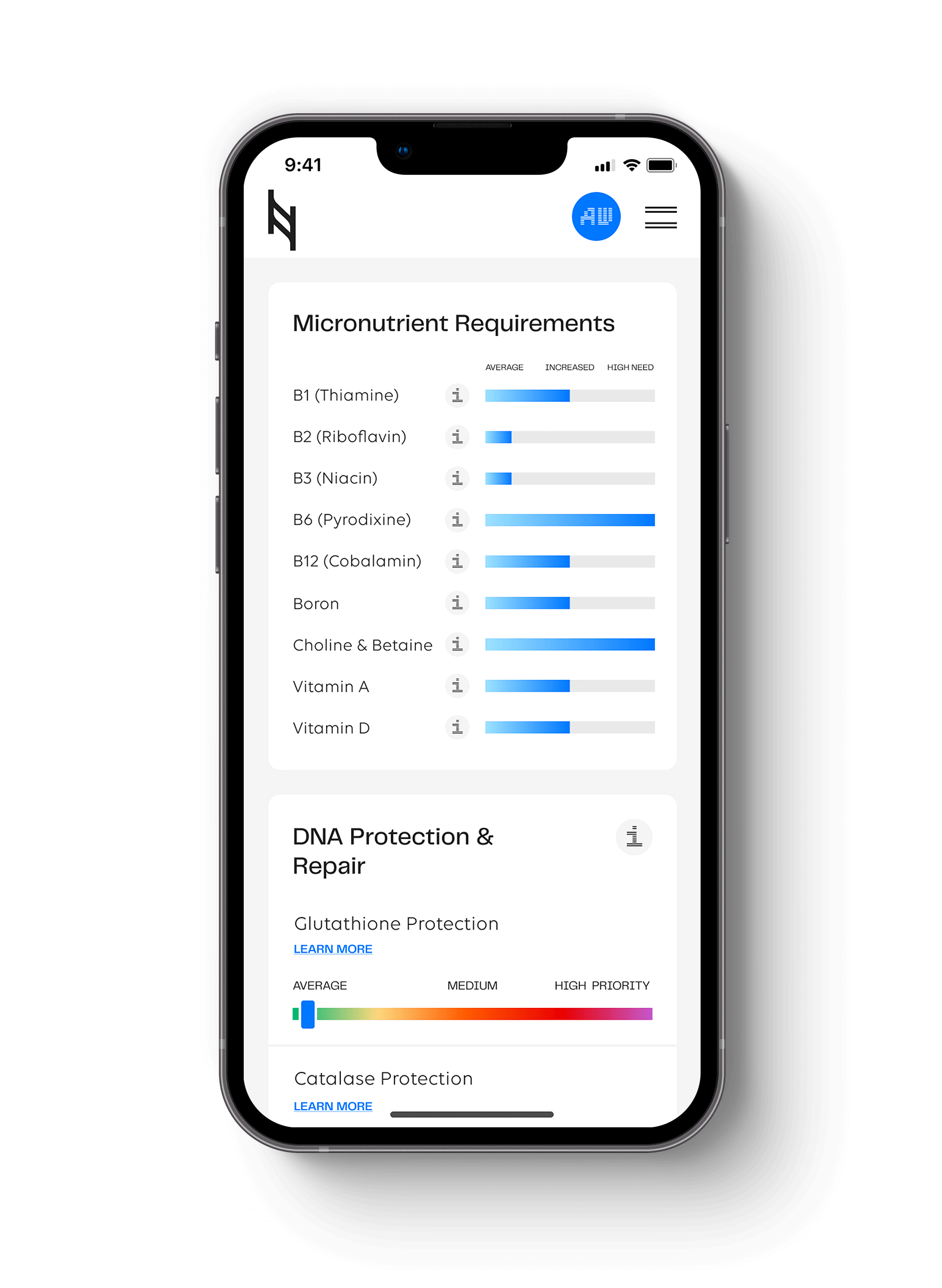
When reviewing the Nutrition Genome Report, genes connected to micronutrient and phytonutrient intake may need to be targeted to help offset the higher risk of skin cancer in your families.
The MTHFR Gene
One hypothesis for why variants occur in the MTHFR 677 gene is due to environmental selection based on higher folate intake and UV exposure, both common in Mediterranean climates. In contrast, the wild-type genotype is most common in Northern climates. Variants reduce MTHFR enzymatic function, increasing the need for folate and increasing thymidine. Thymidine enhances the repair of UV-induced DNA damage to help quickly repair sun damage.
When looking at the statistics, the incidence of malignant melanoma varies from 0.003% to 0.005% per year in Mediterranean countries, and from 0.012% to 0.020% per year in Northern European countries.
Despite lower UV exposure, we see higher rates of melanoma in Northern Europe. The hypothesis is that increased mobility to tropical vacations for those with fair skin starting early in life increases the risk of skin cancer from acute exposure to high UV radiation.
UV radiation depletes folate, and high UV exposure combined with inadequate folate intake and light skin pigmentation could increase the risk of skin cancer in each genotype.
In a 2022 study in Australia, researchers discovered that squamous cell carcinoma risk was modified based on the MTHFR genotype and leafy green intake. For heterozygous and homozygous carriers of MTHFR 677, squamous cell carcinoma risk was lower in the high leafy green intake group than in the low intake group with the same genotype.
The GPX1 Gene
GPX1 activity is considered to be the most critical antioxidant enzyme defense mechanism in the skin. In a study from the Journal of Dermatological Science, the homozygous genotype for GPX1 rs1050450 was associated with a two-fold increased risk of melanoma.
Research has shown that there is reason to believe that individual requirements for selenium will differ because of polymorphisms in seleno-protein genes. In a study looking at a New Zealand population, homozygous carriers of GPX1 rs1050450 had lower GPX1 activity than other genotypes with the same selenium status.
Selenium, cold exposure, optimizing testosterone levels in men and estrogen in women, vitamin C, vitamin E, milk thistle, ginger, cumin, anise, fennel, caraway, and cardamom are all ways to assist GPX1.
Diet and Skin Cancer Risk
When reviewing dietary studies and melanoma risk, epidemiological studies have shown a trend toward reduced melanoma risk with a higher intake of beta-carotene, eggs, legumes, olive oil, vitamins A, C, D, E, fish, fruit, vegetables, and caffeine. Other research has found anti-cancer activity against different types of skin cancer from astaxanthin, lycopene, cordyceps mushroom, green tea, ellagic acid, and citrus peel.
For those with a higher risk of skin cancer, review the modules for micronutrients, phytonutrients, and omega-3s, focusing on vitamin A, C, D, E, folate, choline, selenium, polyphenols, and lycopene. Comparing these requirements with your current dietary and supplement intake can help you customize your program for the highest dietary protection.
Hit your health goals faster
We'll help you remove the guesswork
Experience the most advanced nutrigenomic test available, covering 100 clinically relevant genes for a "whole body" analysis. Take control of your health today.
$359