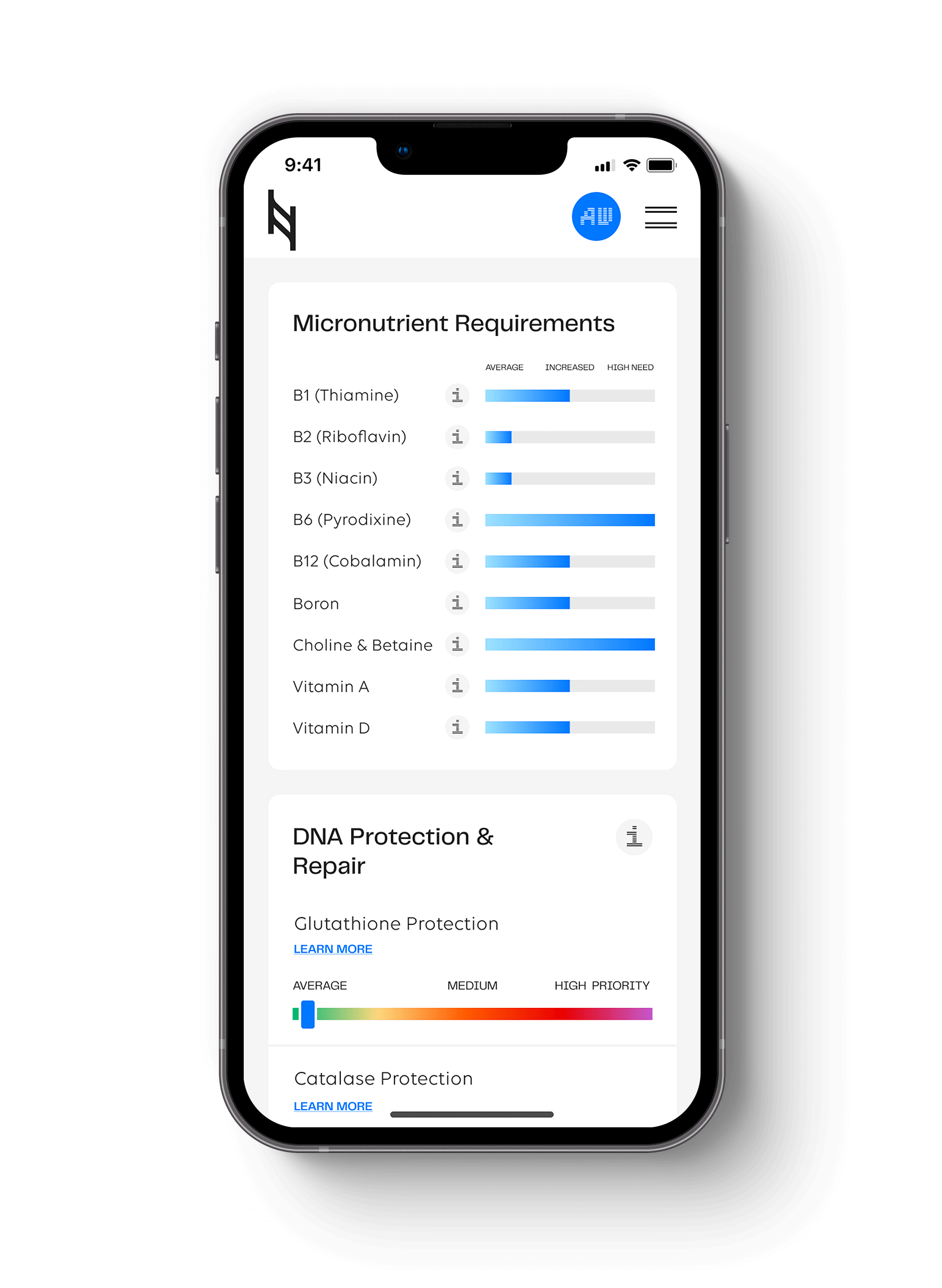
The Nutrition Genome Report looks at multiple genes involved in folate metabolism. which is one of the most relevant parts for fertility and pregnancy. Is the MTHFR gene connected to infertility? Let’s take a look.
The MTHFR Gene and Infertility: The Research
Men with homozygous (C/C) genotype for MTHFR A1298C was present at a statistically high significance for infertility in Moroccan men.
Recently, a meta-analysis was performed in a total of 10 case–control studies, including 2275 cases and 1958 controls; this meta-analysis supports that MTHFR C677T polymorphism is capable of causing male infertility susceptibility in Asians, but not in Caucasians.
A recent study on 151 men with idiopathic infertility and 140 healthy fertile controls of Indian origin concluded that the MTHFR 1298CC genotype is a genetic risk factor for idiopathic male infertility in an Indian population.
A study of 1633 cases and 1735 controls from seven case control studies identified the 1298C allele as a genetic risk factor for infertility, whereas a more comprehensive meta-analyses of 3,850 cases and 4,085 controls from twelve published case–control studies did not observe an association of the 1298C genotype with male infertility, although an association with the MTHFR 677T allele was detected
The researchers conclusion in observing all of this data is that there appears to be a strong connection based on ethnicity and specific phenotybes versus a correlation in every group based only on the genotype.
MTHFR, Folate Status and Infertility
Like MTHFR 677, MTHFR 1298 increases the need for folate. However, the difference appears to be that variants in MTHFR 677 are connected more to homocysteine levels (unless a heterozygous 677 and 1298 are paired), and variants in MTHFR 677 and 1298 may be more sensitive to BH4 levels, where are depleted by toxicty from heavy metals and other factors.
Low levels of folate may negatively impact spermatogenesis by causing DNA hypomethylation, that causes a disruption in gene expression and errors in DNA repair and therefore chromosomal anomalies.
Our hypthosis is that low folate status combined with toxicity is created accelerated DNA damage in the sperm, which is either more pronounced in certain ethnic populations over others, or these populations experience more toxicity depending on the environment.
The Connection to Heavy Metals and Fertility
Lead and Infertility
Lead interrupts the hypothalamic-pituitary axis and has been reported to decrease overall fertility. Lead may alter sperm quality in men, and cause irregular menstruation, induce preterm delivery, and cause miscarriage, stillbirth, and spontaneous abortion in women. Vitamin C lowers lead levels in the body while calcium blocks its uptake, and this may be one of the mechanisms by which vitamin C helps male fertility.
Aluminum and Infertility
Research from scientists in the UK and France suggests that human exposure to aluminum may be a significant factor in falling sperm counts and reduced male fertility. Aluminum in the food supply comes from medications, antacids, water, food additives, and contamination by aluminum utensils and containers.
As one study accurately states “the real scientific question is not the amount of aluminum in foods but the availability of the aluminum in foods and the sensitivity of some population groups to aluminum.”
Mercury and Infertility
Mercury is found in large fish and dental amalgams. Mercury can disrupt spermatogenesis and disrupt fetal development. Folate lowers blood mercury levels, while selenium blocks mercury uptake.
Cadmium and Infertility
Cadmium is another one that should be looked into. It has been shown experimentally to cause testicular necrosis in mice, as well as marked changes in libido and infertility. Non-organic agriculture uses high amounts of synthetic organophosphates which end up in our food, creating a very high phosphorus content. Synthetic phosphorus concentrates the amounts of heavy metals, like cadmium and uranium, in non-organic soils and food.
The researchers in this study conclude “whether it is manufacture or hobby, using any kind of heavy metal or pesticide likely will result in some exposure, and possibly reduce fertility.”
The PON1 Connection to Pesticides and Infertility
The research list on pesticides, herbicides, and other xenoestrogens is very long and convincing. The high concentration of heavy metals in agriculture is especially alarming. Men working in agricultural regions and greenhouses which use pesticides have higher concentrations of common pesticides in their urine and a 60% decrease in sperm concentrations.
Research often focuses on agricultural workers, but it isn’t a far leap to see the ramifications of daily ingestion through chemically grown food and unfiltered water to see how big a deal this is.
People with variants in the PON1 gene may have even more trouble detoxifying these chemicals and require more nutritional strategies including calcium, vitamin E, B1, B2, B5, B6, selenium, omega 3 fatty acids, high-quality olive oil, polyphenols, naringenin, quercetin and moderate exercise.
You can read more about PON1 and the strategies here.
Medications and Infertility
Numerous medications have been linked to infertility, however, it is reversible once stopping the drugs. These include anabolic steroids, antiandrogens, antibiotics, antiepileptics, antihypertensives, anti-inflammatory 5-ASA, antimalarials, antimetabolites, anti-oestrogens, anti-progestins, antipsychotics, antischistosomal, corticosteroids, testosterone, H2 blockers, anaesthetics, methadone, NSAIDs (Advil, Aspirin etc.), Cox-2 inhibitors.
If you are taking any medications that deplete folate, this could compound infertility issues for those with variants in MTHFR.
Hit your health goals faster
We'll help you remove the guesswork
Experience the most advanced nutrigenomic test available, covering 100 clinically relevant genes for a "whole body" analysis. Take control of your health today.
$359